A trial looking at treatment for children and young adults with an ependymoma (SIOP Ependymoma Program II) Pathway 2
Please note - this trial is no longer recruiting patients. We hope to add results when they are available.
Cancer type:
Status:
Phase:
This trial is looking at chemotherapy and extra doses of radiotherapy after surgery to treat ependymoma. It is open to children and young adults with an ependymoma that hasn’t been completely removed by surgery. Cancer Research UK supports this trial.
There are 2 parts to this trial. In the 1st part the trial committee looks at the results of your tests and scans. The 2nd part is looking at treatment pathways.
There are 3 treatment pathways in this trial. This information is about pathway 2. We have information on pathway 1 and pathway 3.
More about this trial
Ependymoma is a type of brain tumour that mostly affects children and young people. We use the term ‘you’ in this summary, but if you are a parent we are referring to your child.
Doctors usually treat ependymoma by removing it with surgery. Afterwards they might give radiotherapy to where the tumour was. Giving chemotherapy before radiotherapy might help those whose tumour wasn’t completely removed by surgery.
In this trial researchers will look at giving the following chemotherapy before radiotherapy
- vincristine, etoposide and cyclophosphamide
- vincristine, etoposide, cyclophosphamide and high dose methotrexate
After this a small amount of tumour might remain. Where possible you have further surgery to remove it. Where this isn’t possible giving 2 more doses of radiotherapy might help.
The aims of this trial are to find
- How well vincristine, etoposide, cyclophosphamide and high dose methotrexate works to treat ependymoma
- How safe the combination is
- What are the side effects of this combination
- How safe it is give 2 more doses of radiotherapy
Who can enter
The following bullet points list the entry conditions for this trial. Talk to your doctor or the trial team if you are unsure about any of these. They will be able to advise you.
You may be able to join this trial if all of the following apply. You
- Have been newly diagnosed with an ependymoma in the brain that is grade 2 or grade 3
- Have had surgery to remove your tumour
- Have had an
MRI scan  after surgery and there is tumour left that cannot be removed by further surgery
after surgery and there is tumour left that cannot be removed by further surgery - Have had an MRI scan and a
lumbar puncture  that shows your tumour has not spread to the spine
that shows your tumour has not spread to the spine - Are able to have radiotherapy and chemotherapy
- Have satisfactory blood test results
- Are willing to use reliable contraception during treatment and for 6 months afterwards if you are sexually active and you or your partner could become pregnant
- Are between 1 year and 22 years old
You cannot join this trial if any of these apply
- You have been diagnosed with an ependymoma called a subependymoma, ependymomablastoma or myoxopapillary ependymoma
- You have already had radiotherapy
- You have already had chemotherapy apart from steroids
- Your ependymoma started in the spine
- You are already having treatment with another anti tumour drug
- You are already taking part in another clinical trial looking at treatment for ependymoma
- You are unable to have any of the drugs used in the trial for any reason
- You have an infection
- There is a medical or another reason why you can’t have the amounts of fluids you need as part of the treatment in this trial
- You have any other medical condition or mental health problem that the trial team think could affect you taking part
- You are pregnant or breastfeeding
Trial design
There are 2 parts to the SIOP Ependymoma Program II.
Part A
In part A you have all the tests and scans that are normally done to diagnose your tumour. A national committee looks at the results of the tests and scans. This is to confirm your diagnosis and consider the most appropriate pathway for you.
The team want to find out more about ependymoma and its treatment. With your permission you will be entered on to a national registry even if you aren’t offered a treatment pathway. They will look at your hospital records to find out what treatment you have.
The trial team need 536 children and young people from the UK and Europe to join part A.
Part B
This is an international phase 2 trial. The researchers need 60 children and young people from the UK and Europe to join.
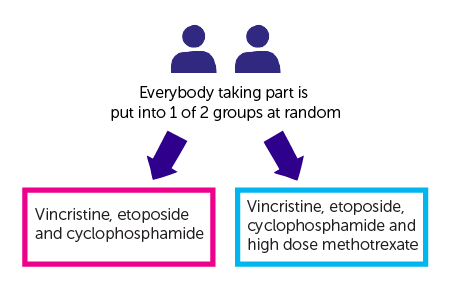
It is a randomised trial. After your surgery you are put into 1 of 2 treatment groups by a computer. Neither you nor your doctor will be able to decide which group you are in
- vincristine, etoposide and cyclophosphamide (group 1)
- vincristine, etoposide, cyclophosphamide and high dose methotrexate (group 2)
Before starting chemotherapy you will have a central line put in. You have all your treatment as a drip through the central line. All blood samples will be taken through the central line.
Group 1
- On the first day of week 1 you have vincristine, etoposide and cyclophosphamide. You then have etoposide for the next 2 days
- Weeks 2 and 3- no treatment
This is repeated 2 more times.
Group 2
- On the first day of week 1 you have vincristine, etoposide and cyclophosphamide. You then have etoposide for the next 2 days.
- During week 2 you have no chemotherapy
- At the start of week 3 you have high dose methotrexate and folinic acid. You have methotrexate over 24 hours through a pump attached to the central line. You have folinic acid for 2 to 4 days afterwards. You have it at regular times as a drip through your central line. Folinic acid helps reduce the side effects of methotrexate
This is repeated 2 more times.
After chemotherapy
You have an MRI scan to see how well the chemotherapy has worked. Any remaining tumour will be removed by surgery if possible. Your doctor will talk to you about this.
Everyone will have radiotherapy. You start radiotherapy 6 weeks after chemotherapy or 6 weeks after surgery.
You have radiotherapy every day Monday to Friday for 6 to 7 weeks. This is the  for ependymoma after surgery. Your doctor will tell you more about it.
for ependymoma after surgery. Your doctor will tell you more about it.
During the last week of radiotherapy you have an MRI scan to see how well it has worked. You will have 2 extra treatments of radiotherapy if there is still some tumour left. This is a booster dose of radiotherapy.
After radiotherapy
You have more chemotherapy to help stop the tumour coming back. This is maintenance chemotherapy.
You start treatment 4 weeks after finishing radiotherapy. The chemotherapy drugs are
- vincristine
- cyclophosphamide
- etoposide
- cisplatin
You have a combination of these drugs at regular times over a period of 16 weeks.
- Week 1 - on the first day of treatment you have vincristine, cyclophosphamide and etoposide. You then have etoposide for the next 2 days
- Weeks 2 and 3 – no treatment
- Week 4 - you have vincristine and cisplatin on the same day
- Week 5 – no treatment
These 5 weeks of treatment is repeated another 2 times. Then you have a
final week of treatment. In this week you have vincristine, cyclophosphamide and etoposide on the 1st day. You then have etoposide only for the next 2 days.
Quality of life study
The trial team will ask you to fill out a few questionnaires
- before you start treatment
- 2 years after your diagnosis
- 5 years after your diagnosis
The questionnaires ask about side effects and how you’ve been feeling. This is called a quality of life study.
For children and teenagers diagnosed under the age of 18 the team will ask you to do the same questionnaires again when you are 18 years old.
Extra tissue and blood samples
With your permission the researchers will ask for a sample of your cancer that was removed when you had surgery. They will also ask to take extra blood and  samples. They will use these samples to find out more about ependymoma. You don’t have to agree to give these samples if you don’t want to. You can still take part in the trial.
samples. They will use these samples to find out more about ependymoma. You don’t have to agree to give these samples if you don’t want to. You can still take part in the trial.
Hospital visits
You see the doctor to have some tests before taking part. These tests include
- A physical examination
- Blood tests
- Urine test
- Lumbar puncture
- MRI scan of the head and spine
- Hearing test
- Tests to see how your brain works (neurological tests)
You might need to stay in hospital for 1 night when the central line is put in.
On the days you have chemotherapy you stay in hospital. Blood tests will be taken regularly. The doctor will see you regularly to see how you are doing.
You see the doctor once a week during radiotherapy for a blood test and physical examination.
After all your treatment has finished you see the doctor
- every 3 months for a year
- every 4 months for the 2nd year
- every 6 months for the 3rd, 4th and 5th year
- then at least once a year until you are 18
At these visits you have
- A physical examination
- Blood tests
- MRI scan
You have a hearing test every 6 months in the 1st year then again at 5 years.
After the age of 18 your doctor will tell you how often they want to see you.
Side effects
The most common side effects of the chemotherapy drugs used in this trial are
- a drop in blood cells causing bruising, bleeding and an increased risk of infection
- feeling and being sick
- loss of appetite
- mouth ulcers
- hair loss
Vincristine can also cause
- tingling in the hands and feet
- changes to the way your kidneys work
- constipation with tummy (abdominal) pains
- nerve pain
- reduced sense of touch
Cisplatin can also cause changes to the way the kidneys work and changes to hearing.
We have more information about the side effects of
We have information about the side effects of radiotherapy to the brain.
Recruitment start:
Recruitment end:
How to join a clinical trial
Please note: In order to join a trial you will need to discuss it with your doctor, unless otherwise specified.
Chief Investigator
Professor R Grundy
Supported by
Cancer Research UK
Centre Léon Bérard
University of Birmingham
Other information
This is Cancer Research UK trial number CRUK/12/036.
If you have questions about the trial please contact our cancer information nurses
Freephone 0808 800 4040



