A trial of radiotherapy and olaparib for cancer of the food pipe (ROCOCO)
Cancer type:
Status:
Phase:
This trial looked at a drug called olaparib alongside radiotherapy for cancer of the food pipe (oesophageal cancer).
Cancer Research UK supported this trial.
The trial was open for people to join between 2013 and 2016. The team reported the results in 2020.
More about this trial
This trial looked at a drug called olaparib. It was for people who couldn’t have surgery or chemotherapy combined with radiotherapy for oesophageal cancer.
The standard treatment at the time for this group of people was radiotherapy on its own. Researchers thought that adding olaparib might make radiotherapy work better but have fewer side effects than adding chemotherapy. They weren’t sure so wanted to find out more.
Olaparib is a type of  called a
called a  . It blocks an enzyme called PARP that cancer cells need to repair themselves and grow.
. It blocks an enzyme called PARP that cancer cells need to repair themselves and grow.
In this trial, some people had radiotherapy and olaparib and some had radiotherapy on its own.
The main aims of the trial were to:
- find the best dose of olaparib to have alongside radiotherapy
- learn more about the side effects
- look at
biomarkers  to understand more about treatment
to understand more about treatment
Summary of results
The trial team didn’t find the best dose of olaparib to have with radiotherapy. The trial closed earlier than planned as it was difficult to find enough people to join.
Trial design
This phase 1 trial ran in the UK. The team had hoped to find about 36 people to join.
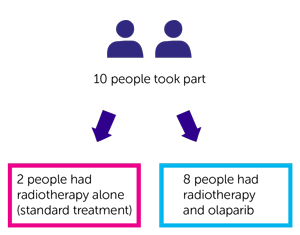
10 people took part. They were put into 1 of 2 groups.
- 8 people had radiotherapy and olaparib
- 2 people had radiotherapy alone (standard treatment). These were people that the trial team didn’t think were suitable for olaparib.
The first few people had a low dose of olaparib. The next few people had a higher dose if they didn’t have bad side effects. And so on, until they found the best dose to give. This is called a dose escalation study.
Olaparib is a tablet. People had it for as long as it was working and the side effects weren’t too bad.
Everyone had radiotherapy from Monday to Friday for up to 5 weeks.
Results
The team looked at the best dose of olaparib to have alongside radiotherapy:
- 5 people had a low dose of olaparib
- 3 people had a higher dose of olaparib
When the team analysed the results, they couldn’t say for sure what the best dose was. They don’t think it was the higher dose. This is because it caused too many side effects. The trial team think the lower dose of olaparib might be safe to give with this type of radiotherapy. But to be sure they would have needed to treat more people and monitor their side effects.
Side effects
The main serious side effects of radiotherapy to the oesophagus and olaparib included:
- weight loss
- difficulty swallowing
- an increased risk of infection
- inflammation of the food pipe
- narrowing of the food pipe (oesophageal stricture)
- a severe breathing problem
One person died as a result of the side effects of their treatment.
Samples for research
Everybody gave some blood and tissue samples ( ) during the trial. The team used the samples to look for substances called
) during the trial. The team used the samples to look for substances called  .
.
Blood samples
The team looked at a marker in the blood called MC65. This was to see if it was possible to use it to monitor how treatment was working. But there was no difference in the level of the marker in those who:
- had the low dose of olaparib with radiotherapy
- had the higher dose of olaparib with radiotherapy
- didn’t have olaparib and had radiotherapy on its own
So the team don’t think that MC65 is a useful marker to see how well treatment is working. There is a small possibility it can be used to work out if the cancer is getting worse.
Skin (tissue) samples
Some people also agreed to have 2 biopsies of their skin. One was from inside the area of radiotherapy, usually from the chest. And one was from the outside, usually from the upper arm. This was to help the researchers understand the effect of the treatment on healthy tissue. The team looked at a marker called GammaH2AX. They compared this marker in those who:
- had the low dose of olaparib
- had the higher dose olaparib
- didn’t have olaparib, just radiotherapy
The team didn’t find a difference in the biomarker levels between the 3 different groups. So they don’t think this was a useful biomarker either.
Conclusion
This was a very small trial. The trial team concluded that they didn’t find the best dose of olaparib to have with radiotherapy to the oesophagus. They think the lower dose could be safe but more people would need to have been recruited to the trial to be completely sure. They thought the higher dose of olaparib definitely wasn’t safe because it caused too many side effects.
Even so, all trial results help doctors and researchers understand more about different cancers and the best way to treat them.
Where this information comes from
We have based this summary on information from the research team. As far as we are aware, the information they sent us has not been reviewed independently ( ) or published in a medical journal yet. The figures we quote above were provided by the research team. We have not analysed the data ourselves.
) or published in a medical journal yet. The figures we quote above were provided by the research team. We have not analysed the data ourselves.
Recruitment start:
Recruitment end:
How to join a clinical trial
Please note: In order to join a trial you will need to discuss it with your doctor, unless otherwise specified.
Chief Investigator
Dr Andrew Jackson
Supported by
AstraZeneca
Cancer Research UK
Experimental Cancer Medicine Centre (ECMC)
NIHR Clinical Research Network: Cancer
The Christie NHS Foundation Trust
Other information
This is Cancer Research UK trial number CRUKD/11/012.
If you have questions about the trial please contact our cancer information nurses
Freephone 0808 800 4040