Treatment
Chemotherapy can work well for some types of brain tumour. But it can be difficult to treat some brain tumours with chemotherapy drugs. This is because the blood brain barrier protects the brain. This is a natural filter and only lets certain substances pass through from the blood to the brain tissues.
Children with a brain tumour might have chemotherapy treatment for up to 18 months.
Your child might have chemotherapy:
after surgery for some types of brain tumour, to try and stop it coming back
with radiotherapy and for some months afterwards
if they have a brain tumour that has come back after treatment
The type of chemotherapy your child has depends on several factors including:
the type of brain tumour
the age of your child
if the tumour is low or high grade
if they’re having an
Children less than 3 years old might have chemotherapy without radiotherapy. It depends on their type of brain tumour. This is to try and avoid radiotherapy to the whole brain and spine when they’re very young. This is to lower the risk of them developing long term side effects. Once they are over 3 years, radiotherapy is used in most children.
Your child’s specialist will discuss the best treatment options for your child with you.
Your child usually has a combination of a few chemotherapy drugs. Here is a list of common chemotherapy drugs used to treat brain tumours:
cyclophosphamide
ifosfamide
vincristine
cisplatin
etoposide
carboplatin
high dose methotrexate
vinblastine
procarbazine
topotecan
dactinomycin
temozolomide
lomustine
thioguanine
irinotecan
methotrexate
We have information about each of these drugs on our cancer drugs A to Z list. The information is based on adults having these drugs. However it can give you a feel of what the side effects may be. If your child has more than one drug, the side effects may be different.
Your child usually has chemotherapy in cycles. This means they have the drugs for a few days every few weeks. There is a time with no treatment when they recover from the side effects.
How often they have treatment depends on the particular drug or drugs they’re having.
Your child might have their chemotherapy as liquid or tablets (oral chemotherapy). Or they might have it through a vein into the bloodstream (intravenous chemotherapy).
Your child usually has treatment through a long flexible plastic tube. This is called a central line. There are different types, including a or . They’re called central lines because they end up in a central blood vessel close to the heart. They run up under the skin to a large vein by the collarbone.
These lines can stay in for much longer than . Sometimes for over 2 years. This means your child doesn’t have to have a cannula each time they have treatment. The nurses can also take blood from these more permanent lines.
We have more information about the different types of central lines. This information is written for adults with cancer, but some of the information and pictures might be helpful.
Some children might have their chemotherapy through a cannula, but this is rare. A cannula is a small tube that is put into your child’s hand or arm.
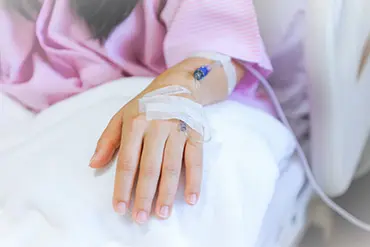
When they aren’t having treatment, your child’s nurse wraps it up with a soft bandage. This is to keep it covered, and prevent your child from taking it out.
During surgery, your treatment team might put a plastic dome under the skin of your child’s scalp. It's called a ventricular access device or an Ommaya reservoir.
Your child’s doctor or nurse gently puts a small needle through your child’s skin into the reservoir. And they give chemotherapy straight into the fluid filled spaces in the brain. So, it goes straight into their cerebrospinal fluid (CSF). This bypasses the blood brain barrier, which means doctors can give smaller doses of chemotherapy.

Chemotherapy travels through the bloodstream to most parts of the body. But, most chemotherapy doesn’t reach the area around the brain and spinal cord well. So, it’s injected into the cerebrospinal fluid to destroy cancer cells in that area.
This is called intrathecal chemotherapy.
Your child’s doctor injects the drug into the fluid around the spinal cord during a lumbar puncture. This diagram shows a girl having a lumbar puncture.

Most children and young people have this test under . Or they might have a medicine to make them feel sleepy and relaxed (). This helps them lie still on the couch for the test.
Side effects vary from one child to another. It is difficult to predict how your child will be and what side effects they will have. Some children have only mild side effects, but for others the side effects are more severe.
Your child’s consultant goes through the benefits and potential side effects of treatment with you. And with your child if they are old enough.
The doctors and nurses looking after your child do everything possible to prevent and treat any side effects that come up. The side effects usually go away quite quickly after treatment stops. But some last longer or start after treatment has finished.
The side effects your child gets might be immediate or long term.
Immediate side effects happen whilst your child is having treatment or very soon after they finish. The side effects depend on which treatments they have. Some common side effects of chemotherapy treatment include:
Increased risk of getting an infection is due to a drop in white blood cells. Symptoms include a change in their temperature, aching muscles, headaches, feeling cold and shivery, and generally unwell. Your child might have other symptoms depending on where the infection is.
Infections can sometimes be life threatening. You should let your child’s doctor or nurse know urgently if you think they have an infection.
Your child might be tired, breathless and look pale due to a drop in red blood cells. This is called anaemia.
This is due to a drop in the number of platelets in their blood. These blood cells help the blood to clot when we cut ourselves. Your child may have nosebleeds or bleeding gums after brushing their teeth. Or you may notice lots of tiny red spots or bruises on their arms or legs (known as petechiae).
Your child might lose all their hair. This includes their eyelashes, eyebrows, and if they have any, under their arms or on their legs. Their hair will usually grow back once treatment has finished, but it is likely to be softer. It may grow back a different colour or be curlier than before.
Constipation is easier to sort out if it’s treated early. If you notice your child isn’t going to the toilet like they were before, let the nurse or doctor know. Try to encourage them to drink plenty and eat as much fresh fruit and vegetables as they can. The doctor may prescribe a laxative to help them.
Your child is likely to feel very tired and lack energy. Work at their pace. Try to get a structure to the day so they don’t nap too often, or they will get their days and nights mixed up. Encourage them to get dressed. Get the play specialist on the ward to help you with a gentle day plan that allows rest.
Your child might feel or be sick. The doctors and nurses usually try to keep it well controlled with regular anti sickness medicines. Try avoiding giving your child fatty or fried foods. Get them to eat small meals and snacks. Encourage them to drink plenty of water and try relaxation techniques to help.
It is important to encourage your child to take anti sickness medicines as prescribed, even if they don’t feel sick. It is easier to prevent sickness rather than treating it once it has started. Some children might need a feeding tube, known as a nasogastric tube.
Your child’s healthcare team will talk you through the medicines they need to take, and if they need a feeding tube.
Chemotherapy treatment can cause mouth sores and ulcers. This can be painful and you might find your child won’t drink or eat normally.
Try to keep their mouth and teeth clean; get them to drink plenty; avoid giving them acidic foods such as oranges, lemons and grapefruits; keep their mouth moist and tell your child’s doctor or nurse if you notice any ulcers or they are struggling to eat and drink.
Some children might have an allergic reaction to some of the chemotherapy drugs. This reaction is likely to happen during treatment or when they first have the treatment. Symptoms of an allergic reaction include high temperature (fever), chills, feeling or being sick and difficulty breathing.
Tell your child’s nurse straight away if you think they have any symptoms of an allergic reaction. They can give them medication to stop this happening.
Some children with a brain tumour develop longer term effects of treatment. These might be from chemotherapy or from a combination of treatments. Long term side effects might develop weeks, months or years after treatment has ended.
These are different for every child. But some possible long term side effects of chemotherapy include:
not being able to have children (fertility problems)
thinning of the bones ()
changes in how the kidneys and heart work
growth problems
a risk of developing a second cancer
hearing problems
Your child’s doctor will talk to you about the possible risks depending on the treatment your child has had. They will continue to keep a close eye on your child, so that any problems can be treated early.
Read about long term side effects and what help and support is available
This page is due for review. We will update this as soon as possible.
Last reviewed: 19 Dec 2022
Next review due: 19 Dec 2025
The main treatments for children’s brain and spinal cord tumours are surgery, radiotherapy and chemotherapy.
Radiotherapy is a common treatment for children’s brain tumours. Find out what type of radiotherapy they might have, what happens before, during and after radiotherapy.
Surgery is a common treatment for a brain tumour. Find out why your child has surgery, who does it and other information.
Brain tumours and their treatment can cause physical and mental changes. Understanding about what they might be can help you cope.
Many children and young people with brain tumours have their treatment as part of a clinical trial. Read about some of the research happening in the UK.
It is essential that parents and other close family have support. Find out what is availble and who can help.

About Cancer generously supported by Dangoor Education since 2010. Learn more about Dangoor Education
Search our clinical trials database for all cancer trials and studies recruiting in the UK.
Connect with other people affected by cancer and share your experiences.
Questions about cancer? Call freephone 0808 800 40 40 from 9 to 5 - Monday to Friday. Alternatively, you can email us.