Living with bladder cancer
You might have a urostomy after surgery to remove your bladder (cystectomy).
You will need to learn how to look after it before you leave the hospital. The nurses and your stoma nurse can show you how to do it.
Read about having surgery to make a urostomy
A stoma is an opening on your . There are different types of stomas. A urostomy is a new way for you to pass urine. Your urine passes through the stoma and collects in a bag on the outside of your body.
Stoma nurses have experience in looking after different types of stomas. They help, support and teach you how to look after yours.
You might see your stoma nurse before your operation. They will show you the different types of you can use. They might give you a stoma kit to practice on first.
After your operation, your nurse will change your urostomy bags. This is until you can change them yourself. Your nurse will show you how to:
clean your stoma
change the bag
empty the bag
Before you leave the hospital, you'll get some urostomy bags to take home. They will also set up an ordering system for you to get the bags from a specialist delivery service. Or they may give you a prescription card to take it to your GP with the details of all the equipment you need.
After you leave the hospital, your stoma nurse might visit you at home to make sure that you are coping. Or you may have a community nurse visit instead. Do ask for their help with any questions or difficulties you have. You’ll have the contact details of your nurse to contact if you have any issues or questions whilst you’re at home.
Most stoma care services have support in place for long term . And patients are easily able to contact them if they get new problems. This is because the aftercare is different after you have surgery compared to a year later.
There are 2 main types of urostomy bags:
1 piece system
2 piece system
Your stoma nurse will help you to find out which system is best for you. The bags are very flat and do not smell or rustle as you move around.
Under ordinary clothes no one can tell you are wearing one. The bag can stay in place for a few days at a time. It has a tap at the bottom so you can empty it into the toilet.
The 1 piece system has the bag, seal and adhesive patch. It can last for up to 3 days. However it is advised to change the patch daily.
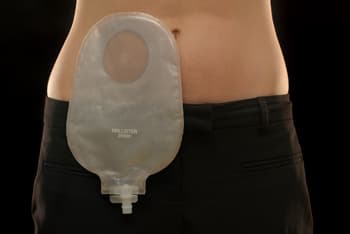
The 2 piece system has a separate bag and adhesive wafer (flange).
The wafer is a soft, flat, plastic adhesive disc that sticks to the body. The bag clips or sticks onto the wafer. You can leave the wafer in place for up to 5 days and just change the bag every 2 to 3 days. However it is advised to change the wafer every 2 to 3 days, and the bag everyday or every other day.
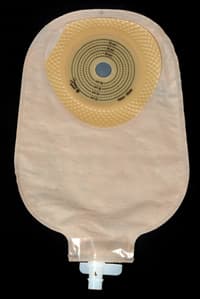
Stoma appliances help you care for your stoma, such as urostomy bags and .
Find a stoma appliance supplier
To fit a new bag, at first you need to cut a hole in the wafer or adhesive patch to fit your stoma. This can feel daunting, so before you go home your nurse will give you a supply of pouches which have already been cut to size. When your stoma has settled in size, you can get bags that are pre cut to fit.
The more accurate the fit, the less likely the bag is to leak. You get very good at this with practice.
What you need:
your new bag and wafer (if you use one)
a measuring guide or the backing film of a pouch as a template
tissues or absorbent cloth
warm water and wipes
a disposal bag or newspaper
scissors
a small mirror for looking at your stoma
a jug to empty the contents of the bag you are wearing or a toilet
You may also need adhesive paste if you're changing your wafer or one piece bag. Or a barrier cream if you have any skin damage.
It’s helpful to keep everything that you need in a bag or in one place. That way, you won't be halfway through and realise something important is missing.
Your stoma nurse will show you how to change your bag. They make sure you know how to do it before you leave the hospital.
Changing your bag can be difficult at first. With practice you start to learn what you need and what works best for you. It helps if your partner or someone close to you understands how to manage a urostomy too.
When changing your bag you don't have to worry about keeping everything sterile. This means keeping it completely free of all germs. But you should be as hygienic as possible.
You should:
wash your hands
cut a hole in the wafer to fit your stoma if it hasn't already been pre cut
make sure the tap is closed on the new bag
drain your old bag
peel the old bag off carefully - you can use an adhesive remover to help with this
throw the bag away in your disposal bag or wrap it in newspaper
clean round your stoma with warm water and wipes
dry the skin thoroughly with tissues or absorbent cloth
if you use barrier cream, massage it in well or it might stop your bag sticking to your skin properly
check the size of your stoma with the measuring guide to make sure it hasn't changed - your stoma nurse will show you how to do this
peel off the paper from the flange
stick your new bag or wafer in place
press down on the flange with warm fingers for 5 to 10 minutes to make sure its sealed to your skin and there are no creases
place your rubbish in the bin
wash your hands
Some organisations can give you advice and support. For example, the Urostomy Association.
The Urostomy Association can arrange for you to meet with other people with urostomies. Members can visit you before and after your operation to support you and give advice on how to cope.
Meeting someone who has been through a similar experience might help you to cope. They know what is important to tell you. And they can answer your questions from first hand experience.
Find out more about the Urostomy Association
Last reviewed: 25 Sept 2025
Next review due: 25 Sept 2028
A urostomy means that you have a bag outside your body to collect your urine. It is also called an ileal conduit.
After surgery to remove your bladder, you will learn to adapt to a new way of passing urine. This can affect your day to day life.
Coping with bladder cancer can be difficult. There are things you can do and people who can help you to cope.
There are organisations and support groups to help you cope with bladder cancer and its treatment.
Bladder cancer is cancer that starts in the lining of the bladder. The bladder is part of the urinary system, which filters waste products out of your blood and makes urine. Find out about the symptoms, how you are diagnosed, treatment, living with bladder cancer and follow up.

About Cancer generously supported by Dangoor Education since 2010. Learn more about Dangoor Education
Search our clinical trials database for all cancer trials and studies recruiting in the UK.
Connect with other people affected by cancer and share your experiences.
Questions about cancer? Call freephone 0808 800 40 40 from 9 to 5 - Monday to Friday. Alternatively, you can email us.