Radiotherapy
Stereotactic radiotherapy gives radiotherapy from many different angles around the body. The beams meet at the tumour. This means that the tumour receives a high dose of radiation and the tissues around it receive a much lower dose. This lowers the risk of side effects.
You usually have treatment through a machine called a linear accelerator (LINAC). But you may also have it on a CyberKnife or GammaKnife machine.

You might hear the term stereotactic radiosurgery. This isn’t a type of brain surgery. It means having a very high dose of stereotactic radiotherapy to a small area. You usually have a single treatment.
Stereotactic radiotherapy and radiosurgery isn’t suitable for everyone. You might have this type of treatment if you have a:
vestibular schwannoma
meningioma
pituitary gland tumour
cancer that has spread to the brain from somewhere else in the body (secondary brain tumour)
You are most likely to have it for small tumours that measure less than 3 cm across.
Secondary brain tumours are different from primary brain tumours. We have separate information about secondary brain tumours.
Find out more about secondary brain tumours
The full dose of stereotactic radiotherapy treatment is usually divided into smaller doses called fractions. The number of fractions you have can vary from between 2 and 5. You have one treatment (fraction) a day.
For radiosurgery, you usually have a single treatment (fraction).
Your head needs to be kept as still as possible during radiotherapy. This is so the treatment is as accurate as possible. Keeping the head still is called immobilisation. So, before you start radiotherapy you have a radiotherapy mask made or a head frame fitted.
Most people have a radiotherapy mask made from plastic. It is called a thermoplastic mask. The mask attaches to the scanner or radiotherapy machine while you are wearing it. This means that you can't move your head.
You have a head frame fitted if you are going to have treatment from a GammaKnife machine.
Your treatment team attaches a frame to your skull using 4 pins. Before they attach the frame, you have injections of local anaesthetic so that you don’t feel any pain. As the frame is fitted, you might feel some pressure and tightness, but it usually feels better within a few minutes.
The treatment team removes the frame when your treatment finishes.
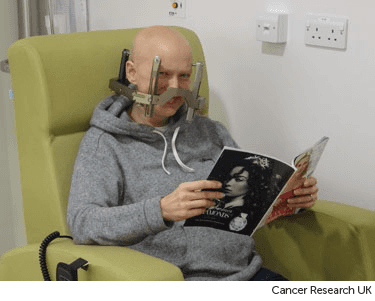
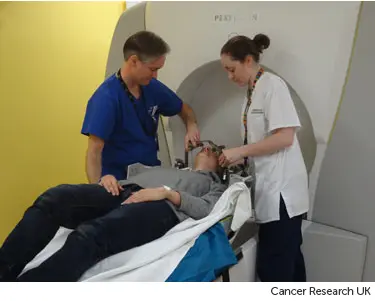
Before treatment, you also have a planning CT scan. This helps your doctors map where the radiation needs to go.
Read about having a planning CT scan and a radiotherapy mask or frame fitted
Radiotherapy machines are very big and could make you feel nervous when you see them for the first time. The machine rotates around you to give the treatment. But it doesn't touch you at any point.
Before your first treatment, your radiographers will explain what you will see and hear. In some departments, the treatment rooms have docks for you to plug in your music player. So you can listen to your own music.
To have treatment you lie on the treatment table. Because your position is so important, the radiographers may take a little while to get you ready. The radiographers attach your mask or head frame into the treatment table. They then leave the room before your treatment starts. This is so they are not exposed to the radiation.
Your radiographers watch and listen to you on a CCTV screen in the next room. Tell them if you need to move or want the machine to stop.
You need to lie very still. The machine makes whirring and beeping sounds. You can't feel the radiotherapy when you have the treatment.
When the treatment is over, the radiographers help you out of the machine. They remove the mask or the frame and you can go back home or to the ward.
This type of radiotherapy won't make you radioactive. It's safe to be around other people, including pregnant women and children.
You might have to travel a long way each day for your radiotherapy. This depends on where your nearest cancer centre is. This can make you very tired, especially if you have side effects from the treatment.
You can ask your radiographers for an appointment time to suit you. They will do their best, but some departments might be very busy. Some radiotherapy departments are open from 7 am till 9 pm.
Car parking can be difficult at hospitals. Ask the radiotherapy staff if you are able to get free parking or discounted parking. They may be able to give you tips on free places to park nearby.
Hospital transport may be available if you have no other way to get to the hospital. But it might not always be at convenient times. It is usually for people who struggle to use public transport. Or who have any other illnesses or disabilities. You might need to arrange hospital transport yourself.
Some people are able to claim back a refund for healthcare travel costs. This is based on the type of appointment and whether you claim certain benefits. Ask the radiotherapy staff for more information about this and hospital transport.
Some hospitals have their own drivers and local charities might offer hospital transport. So do ask if any help is available in your area.
Stereotactic radiotherapy and radiosurgery have fewer side effects than the standard type of external radiotherapy. This is because the area treated is smaller and so less healthy brain tissue is exposed to radiation.
You might feel tired for some time after treatment. But there are other possible side effects.
Find out about the side effects of radiotherapy
This page is due for review. We will update this as soon as possible.
Last reviewed: 05 Apr 2023
Next review due: 05 Apr 2026
Your radiotherapy treatment plan is individual to you. Your radiotherapy team carefully work out how much radiation you need and exactly where you need it.
Radiotherapy to the brain and spinal cord can cause side effects. These include tiredness and feeling sick.
It can be difficult to find out that you have a brain tumour. There is practical and emotional support available to help you, your family and your friends cope with a brain or spinal cord tumour.
Primary brain tumours are cancers that start in the brain.
Survival depends on different factors such as the type, position and grade of your brain or spinal cord tumour.
Primary brain tumours are cancers that start in the brain. Tumours can start in any part of the brain or related structures.

About Cancer generously supported by Dangoor Education since 2010. Learn more about Dangoor Education
Search our clinical trials database for all cancer trials and studies recruiting in the UK.
Connect with other people affected by cancer and share your experiences.
Questions about cancer? Call freephone 0808 800 40 40 from 9 to 5 - Monday to Friday. Alternatively, you can email us.