Treatment
Induction treatment is also called remission induction. In remission means there is no sign of the leukaemia in your child’s blood or when looked at with a microscope.
Induction treatment takes around 4 weeks. Your child is usually in hospital for the first week or two so the nurses and doctors can monitor them closely for any side effects. You can stay with them on the ward. If they are well enough they can go home and then return to the hospital for the rest of their induction treatment on the daycare unit.
Exactly what type of induction treatment your child has depends on a number of things, these include:
their age
if they have T cell or B cell leukaemia
if there are any changes to the leukaemia cells
the amount of leukaemia in the blood
how the leukaemia is responding to treatment
if they have Down syndrome
We have information on how doctors make decisions about treatment for childhood ALL
Before your child starts induction treatment they might have or . They have these because the leukaemia cells are stopping the bone marrow producing normal . They usually have transfusions at the same time as they have tests.
Your child will also have fluids as a drip into their bloodstream (intravenously). And a medicine to protect their kidneys from chemicals released from the breakdown of the leukaemia cells.
They might also need intravenous antibiotics because they don’t have enough healthy to fight infections.
Once the doctors have all the test results they can plan your child’s treatment.
Your child will start induction treatment based on their risk group.
The main treatments are:
chemotherapy
steroids
asparaginase
a targeted cancer drug called imatinib a type of leukaemia called Philadelphia positive leukaemia ALL (Ph+ ve ALL) or for those with a change to the ABL gene
Your child will have a number of drugs over a few days. And it’s likely they will have intravenous fluid too.
Chemotherapy means using anti cancer drugs to destroy cancer cells. But it can also affect normal cells, which can cause side effects.
We have more information on what chemotherapy is here
The drugs your child is most likely to have include:
vincristine
asparaginase – given into a large muscle, such as the upper leg
dexamethasone (a steroid)
intrathecal methotrexate – chemotherapy injected into the fluid around the spine and brain
You can search for each one on our A to Z list of cancer drugs
Some children will also have daunorubicin depending on their induction risk group.
Children with a type of leukaemia called Philadelphia positive ALL or for those with a genetic change to the ABL gene also have a targeted cancer drug called imatinib during induction. Your child usually starts this on day 15 of their treatment.
Your child might need other treatment alongside their treatment for ALL. These are called supportive care medicines. These are different for every child but might include:
medicine to protect their tummy from the side effects of steroids
anti sickness drugs
medicine to reduce the risk of an infection with a type of bacteria that causes pneumonia. This drug is called co-trimoxazole (Septrin)
medicine to protect your kidneys
mouthwashes to help with the side effects of ulcers and sores in the mouth
antibiotics, antifungals and antivirals to help prevent infection
The nurses on the ward give most of your child’s chemotherapy through a vein. At first, the nurses give the chemotherapy through a cannula. This is a small tube that is usually put into your child’s hand or arm.
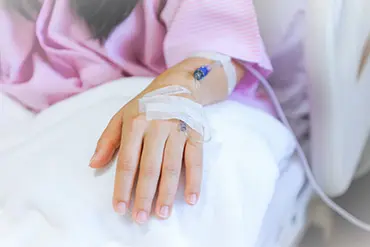
When they aren’t having treatment, your child’s nurse wraps it up with a soft bandage so it’s covered and your child can’t take it out.
Your child has further treatment through a long flexible plastic tube called a central line. They are called central lines because they end up in a central blood vessel close to the heart. They run up under the skin to a large vein by the collarbone.
There are different types of central lines. Your child has the central line that goes into their body in the centre of their chest. The only bit you can see is the length of line that hangs out of the small entry hole in the skin on their chest. This is a picture of a central line in place.
Or they may have another type of central line called a port-a-cath. This is a small chamber or reservoir that sits under your child's skin. It’s attached to a long plastic tube that goes into a large vein close to their heart.

Another type of central line your child might is called a PICC line.
Central lines can stay in for much longer than cannulas. Sometimes for over 2 years. This means your child doesn’t have to have a cannula each time they have treatment. The nurses can also take blood from these more permanent lines.
We have more information about the different types of central lines. This information is written for adults with cancer, but some of the information and pictures might be helpful.
Find out more about having treatment into a vein
Chemotherapy travels through the bloodstream to most parts of the body. But most chemotherapy doesn’t reach the area around the brain and spinal cord well. So, it’s injected into the to destroy cancer cells in that area. This is called intrathecal chemotherapy.
Your child usually has methotrexate chemotherapy this way. Some children might have a chemotherapy drug called cytarabine.
Steroids is another drug that your child might have into their spine.
Go to our cancer drugs A to Z list to find out more about these drugs
Your child has intrathecal chemotherapy or steroids in the same way they have a lumbar puncture.
You can find out more about how your child might have this from the tests page
Steroids are naturally made by our bodies in small amounts. They help to control many functions. But steroids can also be made artificially and used as drugs to treat ALL.
Your child usually has a type of steroid called corticosteroids. These are man-made versions of the hormones produced by the just above the kidneys.
Corticosteroids include:
prednisolone
dexamethasone
methylprednisolone
hydrocortisone
A few children may start taking steroids for up to a week before they start induction treatment. This is usually for those who are quite poorly. The steroids help start to get rid of some of the leukaemia cells while your child’s doctor gets all their test results and plans their treatment.
Asparaginase is a type of chemotherapy drug. Your child will have 2 doses, usually on day 4 and day 18 of their induction treatment.
All cells need a substance called asparagine to make proteins and create new cells. Asparaginase is an enzyme that breaks down asparagine. Unlike normal cells, ALL cells are unable to make their own asparagine. So asparaginase stops the cancer cells from dividing and growing.
Find out more about having asparaginase
The impact of the side effects from of chemotherapy is individual to each child. Your child’s consultant will go through the benefits and potential side effects of treatment with you. They will also go through these with your child if they are old enough.
The doctors and nurses looking after you and your child do everything possible to prevent and treat any side effects that come up. The side effects usually go away quite quickly after treatment stops. But some last longer or start after treatment has finished.
Common short term side effects of chemotherapy include:
increased risk of getting an infection due to low levels of in the blood
anaemia due to low levels of in the blood
increased risk of bleeding due to low levels of in the blood
changes to the levels of chemicals in the blood due to the breakdown of cancer cells (tumour lysis syndrome)
hair loss
diarrhoea or constipation
tiredness and weakness
feeling or being sick
mouth sores and ulcers
allergic reactions
blood clots in the head usually causing headaches
fits (seizures)
Steroids can also cause side effects. Some of the short term side effects include:
changes in blood sugar levels
increased appetite
high blood pressure
mood changes
difficulty sleeping
swollen hands and feet
difficulty walking
Your child being unwell and staying in hospital for the first time can feel overwhelming and scary. Everyone reacts to this differently. There’s no right or wrong way to feel.
One parent or carer can usually stay with your child while they are in hospital. There’s often a bed so you can sleep next to them. There is usually somewhere for you to have a shower and wash your clothes. And a kitchen where you can prepare drinks and snacks.
Hospital wards can often be busy and noisy places, but at night the staff try and keep things as quiet as possible. They need to check on your child throughout the night so it’s easy to get tired through worry and lack of sleep. Try taking it in turns with another family member if that’s possible. It’s important that you get some rest too if you can.
Everyone in the UK has the right to take a reasonable amount of unpaid time off work to look after dependants in an emergency. There’s no set amount of time as it depends on the situation.
Talk to your employer as soon as you feel able to do so, to find out what flexible working arrangements they can offer. It can be hard but try not to rush into any decisions when you are in shock about your child’s diagnosis.
Macmillan have information on your rights at work and what to do if you feel your employer is not being reasonable.
Get information about your rights here on the Macmillan website
Young Lives vs Cancer has a guide for employers on their website. It is about supporting someone whose child has cancer.
Find out more here on the Young Lives vs Cancer website
Carers UK have factsheets and information about your rights in work.
Coping and caring for your other children is difficult when your child is unwell and having treatment. And arranging childcare for your other children can be difficult. You are likely to need to be in hospital with your child during induction as well as other times during the rest of their treatment. This might be because they have an infection or side effects of treatment.
There are organisations that can help you. Talk to your clinical nurse specialist or social worker about what support there might be in your area.
The Rainbow Trust provides support for families of children with a life threatening or terminal illness in certain areas of the UK. Their family support workers support families at home, out in the community and in hospital.
Visit their website to find out more
Going home for the first time after your child has been diagnosed with ALL can feel scary. There is lots of support available, so you won't be alone. Your child’s team will tell you exactly what to look out for, who to call and where to go if your child becomes unwell.
It’s important you take your child to see a doctor straightaway no matter what time of day it is if:
you think they have an infection
they are unwell
you’re worried about them
Infection is one of the key things to look out for with your child when they are at home. This is because their treatment can lower their ability to fight them. Some infections can be life threatening. Although temperature is an important sign of an infection, some children might not get a temperature with their infection. So you should still speak or take them to their doctor if they are unwell or you’re worried.
Here is a list of some symptoms that might mean they have an infection:
feeling generally unwell
a change in breathing, they might get short of breath, find it difficult to breath or develop a cough or wheeze
pain, redness, discharge, swelling or heat at the site of a wound or intravenous line such as a central line or PICC line
they may feel cold, shiver or shake
their appearance may have changed – they may be paler, blotchy or mottled looking
they may go to the toilet more or less than usual, complaining that it hurts when they wee or poo, or you might notice blood in their wee
they may have sores or ulcers in their mouth or throat preventing them from eating and drinking
a temperature above 37.5°C or below 36°
There are other signs and symptoms of a child having an infection. Call the 24 hour advice line number if you’re in any doubt.
The nurses or the pharmacist on the ward will go through what medicines your child should be taking at home. They will explain why they need to take them and when. You could ask for a reminder table or box if you think remembering them will be overwhelming at first.
If your child has a central line the nurses will give you a safety kit before you leave the hospital. The nurses go through looking after your child’s line and what to do in an emergency. The safety kit should be with your child at all times in case its needed.
Before you leave the ward, make sure you know the answers to these questions.
What am I looking out for to make sure my child doesn’t have an infection?
What should I do if my child has signs or symptoms of an infection?
What else should I be looking out for?
How do I look after my child’s central line? (if they have one)
What medication does my child need? Why do they need it? How long for?
Who do I call, or what shall I do, if my child has any side effects of their medication? Or if I’m worried but it’s not an emergency?
Can my child play with our pets?
Who can come and visit us at home?
When is the next blood test and where?
When is the next central line dressing change and where?
You should get a letter when you leave the ward for the first time. This explains about your child’s diagnosis, their medicines and what the plan is next.
Your child has a to check their measurable residual disease (MRD) at the end of the induction phase. This is a very sensitive test and looks for leukaemia cells in the bone marrow.
Your child’s doctor will plan the next phase of treatment. This is called consolidation 1 treatment. Treatment depends on several factors including:
the results of the MRD test
if there are any gene changes (mutations) to the leukaemia cells
your child’s age
the type of cell the leukaemia started in
if there are leukaemia cells in the fluid around the brain or spinal cord (cerebrospinal fluid)
Go to information about consolidation, delayed intensification and high risk block treatment
Last reviewed: 25 Nov 2024
Next review due: 25 Nov 2027
Find out about what to expect when your child is first diagnosed.
Your child’s treatment is divided into phases. Get information on how doctors decide on treatment for childhood ALL.
It is extremely distressing to find out that your child has leukaemia. Find out about what you can do to help you and your family cope when your child is diagnosed with acute lymphoblastic leukaemia (ALL).
Researchers are looking into new treatments for acute lymphoblastic leukaemia as well as ways to reduce the side effects treatment can cause in children and young people. Find out what research is going on.
The aim of these phases is to further reduce and get rid of any leukaemia cells that may be left in the bone marrow and cerebrospinal fluid (CSF). Find out more about these different phases.
Find out about childhood acute lymphoblastic leukaemia, how it is diagnosed and treated, and resources and organisations that can help you cope.

About Cancer generously supported by Dangoor Education since 2010. Learn more about Dangoor Education
Search our clinical trials database for all cancer trials and studies recruiting in the UK.
Connect with other people affected by cancer and share your experiences.
Questions about cancer? Call freephone 0808 800 40 40 from 9 to 5 - Monday to Friday. Alternatively, you can email us.