Treatment
Unfortunately, radiotherapy cannot cure bile duct cancer. Treatment aims to relieve symptoms and improve your quality of life. This is called palliative treatment. It might help you live longer and be more comfortable even if you cannot be cured.
Read more about palliative treatment for cancer
You might have radiotherapy to relieve symptoms caused by the original cancer in your bile duct. This is called the primary cancer. Symptoms might include pain and feeling or being sick.
You may also have radiotherapy to other areas of the body that the cancer has spread to. This can include the:
lungs
liver
bone
brain
Where the cancer has spread to is called a metastasis or secondary cancer. Unfortunately, having a secondary cancer means the cancer is advanced.
Read more about secondary cancer and its treatment
How often you have radiotherapy depends on what symptoms you have and which part of the body you are having the treatment to.
You might have 1 treatment or a number of treatments. Each treatment is called a fraction. You have one fraction a day. If you are having more than one fraction, you have them over a number of days.
You have radiotherapy in the hospital radiotherapy department. It doesn't hurt, but you may find laying on the radiotherapy couch uncomfortable.
The type of radiotherapy you have depends on which part of the body you are having treated.
You normally have stereotactic radiotherapy (SRT) to help control symptoms caused by the primary bile duct cancer. This is a type of . It gives you radiotherapy from many different angles around your body.
Read more about stereotactic radiotherapy
The type of radiotherapy you have depends on where the bile duct cancer has spread to. You might have SRT or other types of external radiotherapy.
Some people may have for cancer that has spread to the liver.
If the cancer has spread to your brain, you may have whole brain radiotherapy (WBRT). You may also have SRT. When SRT is used to treat cancer in the brain it is called stereotactic radiosurgery.
Read more about radiotherapy to control symptoms of secondary cancer
The radiotherapy team plan your external radiotherapy before you start treatment. This means working out the dose of radiotherapy you need and exactly where you need it.
Your planning appointment takes from 15 minutes to 2 hours.
You usually have a planning CT scan in the radiotherapy department.
The scan shows the cancer and the area around it. You might have other types of scans or x-rays to help your treatment team plan your radiotherapy. The plan they create is just for you.
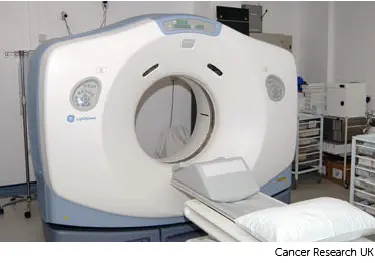
Your radiographers tell you what is going to happen. They help you into position on the scan couch. You might have a type of firm cushion called a vacbag to help you keep still.
The CT scanner couch is the same type of bed that you lie on for your treatment sessions. You need to lie very still. Tell your radiographers if you aren't comfortable.
You might need an injection of contrast into a vein in your hand. This is a dye that helps body tissues show up more clearly on the scan.
Before you have the contrast, your radiographer asks you about any medical conditions or allergies. Some people are allergic to the contrast.
Once you are in position your radiographers put some markers on your skin. They move the couch up and through the scanner. They then leave the room and the scan starts.
The scan takes about 5 minutes. You won't feel anything. Your radiographers can see and hear you from the CT control area where they operate the scanner.
The radiographers make pin point sized tattoo marks on your skin. They use these marks to line you up into the same position every day. The tattoos make sure they treat exactly the same area for all of your treatments. They may also draw marks around the tattoos with a permanent ink pen, so that they are clear to see when the lights are low.

The radiotherapy staff tell you how to look after the markings. The pen marks might start to rub off in time, but the tattoos won’t. Tell your radiographer if that happens. Don't try to redraw them yourself.
You might have to wait a few days before you start treatment. During this time the and your radiotherapy doctor (clinical oncologist) decide the final details of your radiotherapy plan. They make sure that the area of the cancer will receive a high dose and nearby areas receive a low dose. This reduces the side effects you might get during and after treatment.
Radiotherapy machines are very big and could make you feel nervous when you see them for the first time. The machine might be fixed in one position. Or it might rotate around your body to give treatment from different directions. The machine doesn't touch you at any point.
Before your first treatment, your will explain what you will see and hear. In some departments, the treatment rooms have docks for you to plug in your phone or personal device. So you might be able to listen to an audiobook, a podcast or music during the treatment.

The radiographers help you to get onto the treatment couch. You might need to raise your arms over your head.
The radiographers line up the radiotherapy machine using the marks on your body. Once you are in the right position, they leave the room.
You need to lie very still. Your radiographers might take images (x-rays or scans) before your treatment. This is to make sure that you're in the right position. The machine makes whirring and beeping sounds. You won’t feel anything when you have the treatment.
Your radiographers can see and hear you on a CCTV screen in the next room. They can talk to you over an intercom and might ask you to hold your breath or take shallow breaths at times. You can also talk to them through the intercom or raise your hand if you need to stop or if you're uncomfortable.
The short video below shows how you have radiotherapy:
This type of radiotherapy won't make you radioactive. It's safe to be around other people, including pregnant women and children.
You might have to travel a long way each day for your radiotherapy. This depends on where your nearest cancer centre is. This can make you very tired, especially if you have side effects from the treatment.
You can ask your radiographers for an appointment time to suit you. They will do their best, but some departments might be very busy. Some radiotherapy departments are open from 7 am till 9 pm.
Car parking can be difficult at hospitals. Ask the radiotherapy staff if you are able to get free parking or discounted parking. They may be able to give you tips on free places to park nearby.
Hospital transport may be available if you have no other way to get to the hospital. But it might not always be at convenient times. It is usually for people who struggle to use public transport. Or who have any other illnesses or disabilities. You might need to arrange hospital transport yourself.
Some people are able to claim back a refund for healthcare travel costs. This is based on the type of appointment and whether you claim certain benefits. Ask the radiotherapy staff for more information about this and hospital transport.
Some hospitals have their own drivers and local charities might offer hospital transport. So do ask if any help is available in your area.
If you have a short course of radiotherapy treatment of only a few days, you might have very few side effects. You are likely to have more side effects if you have treatment for a couple of weeks.
Side effects tend to start a week after the radiotherapy begins. They gradually get worse during the treatment and for a couple of weeks after the treatment ends. But they usually begin to improve after around 2 weeks or so.
Everyone is different and side effects can vary from person to person. You may not have all of the effects mentioned.
Side effects can include:
tiredness and weakness
feeling or being sick
reddening or darkening of your skin
diarrhoea
loss of body hair
You may have other side effects if you have radiotherapy for a secondary cancer. These can depend on where the cancer is.
You might feel tired during your treatment. It tends to get worse as the treatment goes on.
Various things can help you to reduce tiredness and cope with it, such as exercise. Some research has shown that taking gentle exercise can give you more energy. It's important to balance exercise with resting.
You might feel sick at times. Let your treatment team know if you feel sick, as they can give you anti sickness medicines.
Your skin might go red or darker in the treatment area. You might also get slight redness or darkening on the other side of your body. This is where the radiotherapy beams leave the body.
Radiotherapy to the tummy (abdomen) can cause diarrhoea. Drink plenty of fluids and let your doctor know if you have frequent diarrhoea.
You may lose some body hair in the treatment area. This may grow back a few weeks after treatment finishes. But sometimes it doesn't. Your doctor will talk to you about this before you start treatment.
Last reviewed: 11 Oct 2024
Next review due: 11 Oct 2027
Treatments for bile duct cancers include surgery, chemotherapy and treatments to control symptoms. The treatments you have depend on the stage of the cancer.
Advanced bile duct cancer has spread outside the bile ducts into nearby lymph nodes or organs. Or it has spread to parts of the body further away from the bile ducts.
Your healthcare team can give you medicines to help control some of the symptoms of bile duct cancer. There are also practical things you can try.
You have regular tests and follow ups if you have bile duct cancer, or after surgery to remove the cancer. How often you have the appointments depends on your situation.
Advanced bile duct cancer is cancer has spread outside the bile ducts. It can also mean bile duct cancer that has come back some time after you were first treated. There is support to help you cope. And the symptom control team can help you feel as well as possible.
Bile duct cancer is also called cholangiocarcinoma. It is a rare type of cancer that develops in the small tubes that connect the liver and gallbladder to the small bowel.

About Cancer generously supported by Dangoor Education since 2010. Learn more about Dangoor Education
Search our clinical trials database for all cancer trials and studies recruiting in the UK.
Connect with other people affected by cancer and share your experiences.
Questions about cancer? Call freephone 0808 800 40 40 from 9 to 5 - Monday to Friday. Alternatively, you can email us.