Treatment
External radiotherapy uses a machine outside the body to direct radiation beams at the cancer to destroy it.
Radiotherapy treatment works by damaging the within the cancer cells. DNA is the genetic code that controls how the body's cells behave.
Find out more about external radiotherapy
You might have radiotherapy to:
the whole body (total body irradiation, TBI) as part of conditioning treatment for a .
AML that has formed a lump outside the bone marrow (also known as myeloid sarcoma, granulocytic sarcoma, chloroma or extramedullary myeloid tumour)
the brain or spinal cord if AML has spread there, although it is rare for this to happen
Your healthcare team will explain the type of radiotherapy treatment you will be having.
Find out more about total body irradiation (TBI)
You might have radiotherapy as a single treatment or a series of daily treatment sessions. A single dose of radiotherapy is called a fraction. A series of sessions makes up a radiotherapy course.
The number of treatment sessions you need depends on your situation. Your doctor will discuss with you how many sessions you need.
Conditioning treatment prepares you for a stem cell transplant. TBI is part of the conditioning treatment. The number of radiotherapy fractions you have depends on the type of conditioning you have. For example, for reduced intensity conditioning (RIC) you may have 1 or 2 fractions. With full intensity (myeloablative) conditioning you might have up to 8 treatment sessions over 4 days. So 2 fractions a day.
Find out more about having a stem cell transplant for AML
Before you begin your treatment, the radiotherapy team carefully plan your external beam radiotherapy. This means working out how much radiation you need to treat the cancer and exactly where you need it.
Your planning appointment may take from 15 minutes to 2 hours.
You usually have a planning CT scan in the radiotherapy department.
The scan shows the cancer and the area around it. You might have other types of scans or x-rays to help your treatment team plan your radiotherapy. The plan they create is just for you.
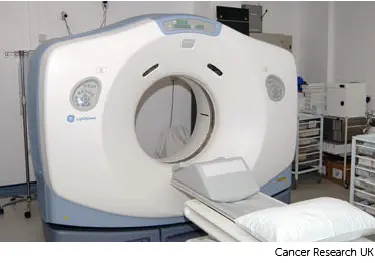
Your radiographers tell you what is going to happen. They help you into position on the scan couch.
The CT scanner couch is the same type of bed that you lie on for your treatment sessions. You have to lie as still as you can, so that the measurements are accurate and the radiographers can record your exact position. This means they can make sure you are lying in the correct position every time you have treatment.
Once you are in position your radiographers put some markers on your skin. They move the couch up and through the scanner. They then leave the room and the scan starts.
The scan takes about 5 minutes. You won't feel anything. Your radiographers can see and hear you from the CT control area where they operate the scanner.
Watch our video about radiotherapy planning, this is just under 3 minutes long.
Depending on why you are having radiotherapy the radiographer might also do some extra things during the appointment. This may include:
making a mould or mask for radiotherapy to the brain
tattooing the skin
The radiographers make pin point sized tattoo marks on your skin. They use these marks to line you up into the same position every day. The tattoos make sure they treat exactly the same area for all of your treatments. They may also draw marks around the tattoos with a permanent ink pen, so that they are clear to see when the lights are low.

The radiotherapy staff tell you how to look after the markings. The pen marks might start to rub off in time, but the tattoos won’t. Tell your radiographer if that happens. Don't try to redraw them yourself.
If you are having treatment to your head you may need to have a mould (shell) made to keep you perfectly still while you have treatment.
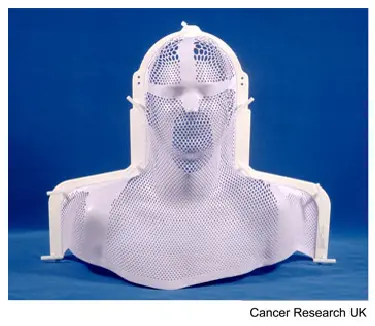
The moulds are made in the mould room or in the CT scanning room.
Read more about radiotherapy masks and moulds
You might have to wait a few days or up to 3 weeks before you start treatment.
During this time the physicists and your radiotherapy doctor (clinical oncologist) decide the final details of your radiotherapy plan.
Then the physicists and staff called dosimetrists plan the treatment very precisely using computers.
Read more about creating your radiotherapy plan
Radiotherapy machines are very big and could make you feel nervous when you see them for the first time. The machine might be fixed in one position. Or it might rotate around your body to give treatment from different directions. The machine doesn't touch you at any point.
Before your first treatment, your will explain what you will see and hear. In some departments, the treatment rooms have docks for you to plug in your phone or personal device. So you might be able to listen to an audiobook, a podcast or music during the treatment.

The radiographers help you to get onto the treatment couch. You usually lie on your back and might need to raise your arms over your head.
The radiographers line up the radiotherapy machine using the marks on your body. Once you are in the right position, they leave the room.
You need to lie very still. Your radiographers might take images (x-rays or scans) before your treatment to make sure that you're in the right position. The machine makes whirring and beeping sounds. You won’t feel anything when you have the treatment.
Your radiographers can see and hear you on a CCTV screen in the next room. They can talk to you over an intercom and might ask you to hold your breath or take shallow breaths at times. You can also talk to them through the intercom or raise your hand if you need to stop or if you're uncomfortable.
This type of radiotherapy won't make you radioactive. It's safe to be around other people, including pregnant women and children after your treatment.
The short video below shows how you have radiotherapy. It’s just over 2 minutes long.
Radiotherapy for AML can cause side effects. These will depend on:
where you are having treatment to
how much radiotherapy you have (the number or fractions and overall dose)
if you have it with other treatments such as chemotherapy
Your healthcare team will explain possible side effects and what to do if you have them.
Radiotherapy general side effects and side effects of radiotherapy to different parts of the body
Last reviewed: 16 Apr 2024
Next review due: 16 Apr 2027
External radiotherapy targets radiation at the cancer from a radiotherapy machine. Read about types of external radiotherapy and what happens during planning.
Radiotherapy to the whole body is called total body irradiation or TBI. You might have TBI as preparation for your stem cell or bone marrow transplant at the same time as high dose chemotherapy and targeted cancer drugs.
Chemotherapy is the main treatment for acute myeloid leukaemia (AML). Find out how your doctor decides your treatment, detailed information about the each treatment, the side effects and follow up.
You might either have a stem cell or bone marrow transplant.
AML starts from young white blood cells called granulocytes or monocytes in the bone marrow. Find out about symptoms, how it is diagnosed and treated, and how to cope.

About Cancer generously supported by Dangoor Education since 2010. Learn more about Dangoor Education
Search our clinical trials database for all cancer trials and studies recruiting in the UK.
Connect with other people affected by cancer and share your experiences.
Questions about cancer? Call freephone 0808 800 40 40 from 9 to 5 - Monday to Friday. Alternatively, you can email us.