Spot cancer early
More people are surviving cancer today than ever before. And thanks to research, treatments are now kinder and more effective than ever. A key part of this progress comes from earlier cancer diagnosis. An ‘early’ cancer diagnosis is when cancer is spotted at an early stage, such as stage 1 or 2, before it has grown too large or spread to other parts of the body.
Find out more about the stages of cancer.
When cancer is found at an early stage, treatment is more likely to be successful. At this point, the cancer is usually small and hasn’t spread. For some cancer types, this can lead to more treatment options. It can also increase the chances of having a local treatment, like surgery, where only a certain area of the body needs treatment. This could be enough to get rid of the cancer completely. Even if cancer has started to spread, detecting it as soon as possible can still make a big difference. Earlier treatment may slow or stop the cancer progressing further. That’s why it’s important to tell your doctor if you notice anything that isn’t normal for you.
Diagnosing cancer earlier makes a difference for most cancer types. But here are a few examples of how spotting cancer early can improve survival for some more common cancers:
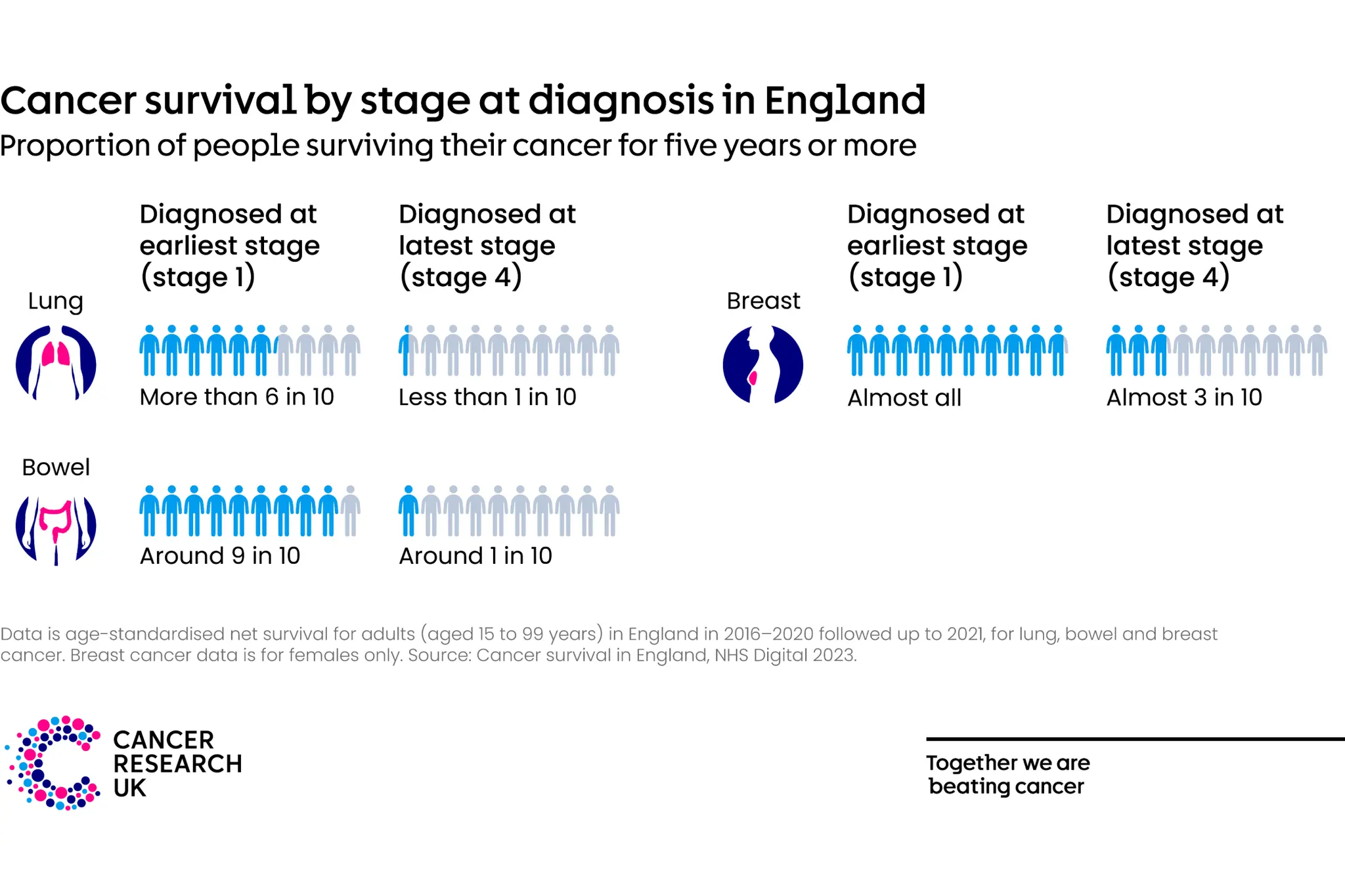
In England, almost all (98%) women with breast cancer survive their disease for five years or more when diagnosed at the earliest stage. This falls to almost 3 in 10 women (27%) when breast cancer is diagnosed at the most advanced stage (2016-2020). *
Find out more about symptoms of breast cancer and breast cancer diagnosis.
In England, around 9 in 10 (91%) people with bowel cancer survive their disease for five years or more when diagnosed at the earliest stage. This falls to 1 in 10 (11%) people when diagnosed at the latest stage (2016-2020). *
Find out more about symptoms of bowel cancer and bowel cancer diagnosis.
In England, more than 6 in 10 (63%) people with lung cancer survive their disease for 5 years or more, if diagnosed at the earliest stage. This falls to less than 1 in 10 (4%) when diagnosed at the most advanced stage. * Lung cancer doesn’t always cause symptoms in its early stages. But speaking to your doctor as soon as possible if you spot anything unusual can still make a difference. Almost 2 in 10 people with lung cancer survive their disease for five years or more when diagnosed at stage 3. Around 4 in 10 people with lung cancer survive their disease for five years or more when diagnosed at stage 2.
Although many of the common symptoms of lung cancer can also be caused by other medical conditions, it’s always best to get checked out. Find out more about lung cancer symptoms and lung cancer diagnosis.
There are lots of factors which can affect how quickly cancer is found. But there are still things you can do which may help detect cancer early.
There’s no specific way you need to check your body for cancer. And what’s normal for one person can be different for another. The best thing you can do is be aware of what your body usually looks and feels like. This can make it easier to spot any unusual changes. If you do notice something that isn’t quite right, listen to your body and get it checked out.
There are over 200 different types of cancer, and they all have different signs and symptoms. You don’t need to remember all the symptoms of cancer. But it’s important to listen to your body. If you notice anything that isn’t normal for you, or if something doesn’t feel quite right, take charge and speak to your doctor. Talk to your doctor again if your symptoms don’t go away or get worse, even if your tests have come back normal or you are waiting to have tests. In most cases it won’t be cancer – but if it is, finding it early can make a real difference. Learn more about the key signs and symptoms of cancer.
In the UK, there are cancer screening programmes for breast, cervical and bowel cancer. Cancer screening is offered to people with no symptoms. It aims to find possible signs of cancer before they are noticeable. Screening can detect cancers at an early stage or in some cases, prevent them from developing in the first place. Find out more about cancer screening, who it’s for, and the UK cancer screening programmes on our cancer screening homepage.
Early diagnosis is important, but it’s not always easy. There can be several reasons why cancer might not be diagnosed early:
Some possible cancer signs and symptoms might not be obvious, such as feeling tired for no reason, or unexplained aches or pains. Some types of cancer may also not show symptoms until later stages.
Not all diagnoses are straightforward. Doctors might investigate other possibilities before making a cancer diagnosis. For some cancers, we need better tools that can spot cancer earlier.
People may put off speaking to a doctor. Worry, embarrassment, or not wanting to bother the doctor can put some people off from seeking help.
It may be difficult to get an appointment. Some people can find it hard get an appointment at a convenient time, or in a place that’s easy to get to. For more information on getting an appointment that works for you, visit our talking to your doctor webpage.
It can sometimes take time to get a referral for tests, or to get an appointment at the hospital.
Thinking about cancer can be worrying. But taking action early can make a real difference. Talk to your doctor if something doesn’t feel quite right – they will want to hear from you.
Our research has already helped more people get diagnosed earlier, when treatment is more likely to be successful. And we’re continuing to work hard to make sure more cancers are detected at an earlier stage. From developing better tools to detect cancer, to identifying people who may be at higher risk, our researchers are developing new ways to help spot cancer early.
Current research includes trialling a ‘sponge on a string’, which detects changes in the food pipe (oesophagus) before they can lead to cancer. And a world-first urine test that could help to detect early signs of lung cancer. We’ve also supported a range of clinical trials that are exploring other methods of spotting cancer early, such as a trial of an early cancer detection blood test. Visit our early diagnosis research webpage for more information about our current and past research.
Alongside research, Cancer Research UK is campaigning to make early diagnosis a priority issue for the UK Government. We’ve seen some positive progress in recent years, including the commitment to introduce a national targeted lung screening programme in England, Scotland and Wales, but more action is needed to ensure as many patients as possible receive an early diagnosis. Read more about our policy calls in our report ‘A full diagnostic’ and our manifesto, ‘Longer, better lives’.
Last reviewed: 13 Feb 2026
Next review due: 13 Feb 2029
Questions about cancer? Call freephone 0808 800 40 40 from 9 to 5 - Monday to Friday. Alternatively, you can email us.