Types of external radiotherapy
Image guided radiotherapy (IGRT) uses scans and x-rays to make sure that you're in the correct position for your radiotherapy treatment. You have them while you are on the radiotherapy couch, just before your treatment starts. Your radiographers check them against the scan you had at your planning appointment.
They might move the radiotherapy couch or your position after looking at the x-rays and scans. This is to make sure you're in a position very close (within millimetres) to your planning scan.
Sometimes you might have an x-ray or scan just after your treatment. You stay in the same position for this and it's used as another check.
X-rays show your bones in the treatment area. And scans show the size, shape and position of the cancer as well as the surrounding tissues and bones.
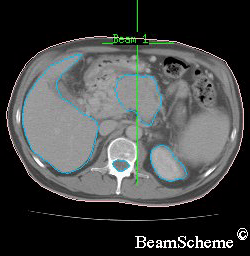
An example of a scan
In some areas of the body, cancers may move slightly during or between treatments. For example, the prostate gland changes position according to whether the bladder is full or not. You might also lie down in a slightly different position each day. So there is a risk that part of the cancer may be outside the treatment area for some treatment sessions.
Taking scans and x-rays just before your treatment, makes sure that you are in a position very close to your planning scan.
If your radiographers see from your first few images that your position is very similar each day, they may not need to take images every day.
4D-RT involves images being taken during your treatment. The radiotherapy machine can then adjust the position of the couch using information from these images.
In some types of 4D-RT the machine may switch off if the cancer moves out of the radiotherapy field. This type of treatment is helpful for cancers in areas of the body that move when we breathe, such as the lungs. The radiation beam switches on again when the cancer moves back into the right position. Your radiographers are always in control of the radiotherapy machine.
Most external radiotherapy machines can deliver IGRT. A linear accelerator (LINAC) is the most common radiotherapy machine.
To have the treatment you lie on a radiotherapy couch. Your radiographers help you to get into the right position. They also put on any radiotherapy moulds or masks.
Read about radiotherapy masks or moulds

Once you are in the right position your radiographers leave you alone in the room. This is so they are not exposed to the radiation but they can see and hear you the whole time.
You can't feel anything when you have the treatment. It doesn’t hurt. It takes between 15 to 45 minutes.
You may have small metal markers (fiducial markers) put in or near your tumour. This is common for prostate cancer.
To place the markers, your doctor inserts a needle into the area of skin over the cancer. They do this while you are having an ultrasound scan. Once the tip of the needle is in the right place your doctor releases small gold pellets or rods.
Your radiographers can then see the markers on x-rays and scans while you're having treatment. They act as a marker for the treatment area, and makes sure that the treatment is very accurate. Your radiographers will take x-rays or scans every day before treatment if you have this type of metal marker.
With IGRT, doctors can target the radiotherapy treatment area very accurately. So that there is less radiation to nearby healthy tissues. This can reduce your chance of side effects from radiotherapy. But taking images during treatment can:
increase the length of time that you're on the radiotherapy couch
be uncomfortable
slightly increase the amount of radiation that you're exposed to
It's important to remember that this is still a very small amount compared to your treatment dose. Your doctor and radiographers make sure the benefits of taking the images outweigh the risks. This is the reason why you might not have scans and x-rays every day.
Last reviewed: 09 Nov 2023
Next review due: 09 Nov 2026
External radiotherapy uses radiotherapy machines to aim radiation beams at a cancer. This destroys the cancer cells. There are different types of external radiotherapy.
You might have radiotherapy to try to cure cancer or to help relieve symptoms. You might have it with other treatments such as chemotherapy or surgery.
Your radiotherapy treatment plan is individual to you. You have a CT scan or MRI scan, to create your radiotherapy plan.
Radiotherapy can cause different side effects depending on which part of the body is being treated. Find out what these side effects are and how they affect you during and after treatment.
Find out about cancer treatment with radiotherapy, including external radiotherapy, internal radiotherapy, side effects, radiotherapy for symptoms and follow up after treatment.
Search for the cancer type you want to find out about. Each section has detailed information about symptoms, diagnosis, treatment, research and coping with cancer.

About Cancer generously supported by Dangoor Education since 2010. Learn more about Dangoor Education
Search our clinical trials database for all cancer trials and studies recruiting in the UK.
Connect with other people affected by cancer and share your experiences.
Questions about cancer? Call freephone 0808 800 40 40 from 9 to 5 - Monday to Friday. Alternatively, you can email us.