Astrocytoma in children
Astrocytomas are the most common type of brain and spinal cord tumour in children. They are also known as a glioma. This is because they develop from a type of glial cell called an astrocyte. There are low grade and high grade astrocytomas (gliomas).
Around 175 children are diagnosed with an astrocytoma each year in the UK.
Children can develop an astrocytoma at any age. Boys and girls are equally affected.
Where do astrocytomas start?
Astrocytomas develop from the cells called astrocytes. Astrocytes are star shaped cells. They support the nerve cells (neurones) in the brain.

Some astrocytomas are very localised (focal). This is also known as circumscribed. This means it is easy to see the border between the tumour and normal brain tissue on a scan or during an operation. These types of tumours are more common in children than in adults.
Other astrocytomas are called diffuse. They don’t have a clear boundary between the tumour and normal brain tissue.
Astrocytomas can start anywhere in the brain and spinal cord including the:
- cerebrum (forebrain)
- cerebellum (hindbrain)
- brain stem
- eyesight nerve pathways (optic nerves)

Risks and causes
We don’t know what causes most childhood cancers, or how to prevent them. This includes astrocytomas.
We know that there is an increased risk of low grade astrocytoma with a genetic condition called  . Around 15 to 20 out of 100 low grade astrocytomas (around 15 to 20%) are linked to NF1.
. Around 15 to 20 out of 100 low grade astrocytomas (around 15 to 20%) are linked to NF1.
Because of this, children with NF1 have regular eye checks. This is to check for any sight problems which a tumour in the eyesight nerve pathway could cause.
Signs and symptoms
Some children may have symptoms for a few weeks or months before they’re diagnosed with an astrocytoma. This is especially true if they have a low grade, slow growing astrocytoma.
Many symptoms are general and non specific. Some are similar to less serious childhood illnesses. Symptoms include:
- headaches in the morning
- feeling or being sick – being sick often makes the headaches feel better
- double vision
- seizures (fits)
Other symptoms depend on where the astrocytoma is in the brain.
Young infants might have an increasing head circumference. A health professional measures this during their well baby check ups. Or the soft spot on top of the skull (fontanelle) might be swollen.
Take your child to the general practitioner (GP) to get checked out if you are worried they have symptoms of a brain tumour.
Tests
The first test your child might have is an  .
.
Your child’s surgeon might take a sample of the tumour (a biopsy) for testing in the laboratory. They take the sample using a needle during an operation.
Your child’s team decides if a biopsy is a safe test, depending on the results of scans. It’s not always possible or necessary to take a biopsy before treatment. This might be due to the position of the tumour in the brain.
For some types of tests, your child might need  or a
or a  . This is to help them lie still.
. This is to help them lie still.
Other tests your child might have include blood tests to check their hormone levels. Some astrocytomas can affect the hypothalamus or  in the brain. Your child’s doctor will explain this to you.
in the brain. Your child’s doctor will explain this to you.
Types and grading of astrocytomas
There are 3 main types of astrocytomas (gliomas) in children. These are:
- circumscribed pilocytic astrocytomas
- diffuse low grade gliomas
- high grade gliomas
The grade of a tumour shows what the cells looks like under the microscope. It shows whether the cells look similar to normal cells or are very different. It gives the doctor an idea of how the tumour might behave. For example if it is slow or fast growing.
Tumour cells that look similar to normal cells are low grade. These tumours grow fairly slowly and are less likely to spread. Tumour cells that are very abnormal looking are high grade. High grade tumours tend to grow more quickly and are more likely to spread to other areas of the brain and body.
Most astrocytomas in children are low grade.
For each main type of astrocytoma, there are several subtypes – some of which include specific genetic information. For example:
- Pilocytic astrocytoma (a type of circumscribed astrocytoma – BRAF KIAA 1549 fusion)
- Diffuse astrocytoma, MYB-or MYBL1-altered (a type of diffuse low grade glioma)
- Diffuse midline glioma, H3 K27-altered (a type of diffuse high grade glioma)
Pilocytic astrocytoma is the most common type of astrocytoma diagnosed in children.
The  of brain tumours is quite complicated. Your child’s doctor or nurse will help explain what type of tumour your child has and what it means.
of brain tumours is quite complicated. Your child’s doctor or nurse will help explain what type of tumour your child has and what it means.
Decisions about treatment
Your child’s specialist team decides on the best treatment options for your child. The team will involve you and your child in the decisions about their treatment and care.
Treatment for astrocytoma in children depends on:
- the grade of the tumour – if it is fast or slow growing
- where the tumour is in the brain
- if it is possible to remove the tumour with surgery
- how old your child is
- if they are having symptoms
Treatment
The main treatments for astrocytomas are:
-
surgery
-
radiotherapy
-
chemotherapy
Your child might have steroids to help reduce swelling in the brain. This is usually a steroid drug called dexamethasone.
If your child is having seizures (fits), they may start on a medicine to stop these. These are called anticonvulsants.
Treatment for low grade tumours
Surgery is the main treatment. Sometimes surgery is not possible. Or the surgeon might not be able to remove all the tumour during the operation.
In this case, the doctors will talk with you about the other treatment options for your child.
The main treatment for most astrocytomas is surgery to remove as much of the tumour as possible. But it isn't always possible to fully remove tumours in some areas of the brain.
For example, surgery to remove tumours in the brainstem can cause too much damage to the surrounding normal brain tissue.
Low grade tumours are generally easier to remove than high grade tumours. This is because they are less invasive. This means they don't spread out into the surrounding brain tissue in the way that some high grade tumours do.
Surgery might be the only treatment your child needs.
Hearing your child needs brain surgery can feel very frightening. A paediatric neurosurgeon does the operation. They are highly skilled professionals. They can help answer any questions you might have about the operation.
Fluid build up
Some tumours whether they are low or high grade cause fluid to build up in the brain. This is called hydrocephalus. Treatment to reduce this is an operation. Your child’s surgeon might:
- make a hole to drain fluid into another area of the brain, where it is absorbed (ventriculostomy)
- put a small tube called a shunt in your child’s brain, so that the fluid drains to another part of the body. This is usually the tummy, where the body gets rid of it
- remove the tumour if it is safe to do so
What if surgery isn’t possible?
Sometimes surgery is not possible because of where the tumour is in the brain. If your child doesn’t have any symptoms, they might suggest that they closely monitor the tumour. This means your child will have regular scans to check for any changes. These types of tumours are slow growing, so might not cause problems for your child for quite a while.
If the tumour is causing symptoms, they might suggest another treatment such as chemotherapy, radiotherapy or a  .
.
Your child’s doctors will talk with you about the other treatment options.
If the surgeon is able to remove most of the tumour your child will be closely followed up. They’re likely to have regular scans, but no further treatment at this stage.
Radiotherapy means the use of radiation, usually with high energy x-rays, to treat cancer. Your child’s team might suggest your child has radiotherapy.
Doctors try to avoid giving radiotherapy treatment to children:
- under the age of 10
- with NF1
This is because they are more at risk of severe side effects during and after treatment.
Proton beam therapy is a type of radiotherapy. It uses protons rather than high-energy x-rays to kill cancer cells. Protons are tiny parts of atoms. They work differently from x-rays. They produce a sudden burst of energy when they stop, which stays inside the tumour. So, there is less damage to healthy cells around the tumour.
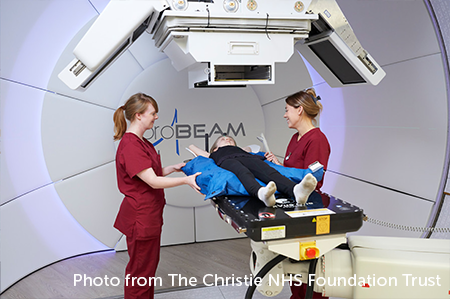
Research shows that proton beam therapy can work well for some types of children’s brain tumours. This includes some children with low grade astrocytoma.
Your child’s specialist will talk with you if proton therapy might be helpful for your child.
There are 2 therapy centres in the UK and these are at:
- The Christie Hospital in Manchester
- University College London Hospital
University College London Hospital opened in 2021. They’re gradually opening their service to the rest of the UK. At the moment, children who need this service will have to travel to one of these hospitals or abroad.
Chemotherapy is the use of anti cancer drugs to destroy cancer cells. Your child’s specialist might recommend chemotherapy instead of radiotherapy. Or your child might have chemotherapy and radiotherapy together.
Your child will have most of their chemotherapy into a vein (intravenous).
Chemotherapy can work very well for some types of astrocytoma in babies and young children. The exact combination of drugs and the timing varies. But generally chemotherapy is given every 2 to 6 weeks. Children under 2 years of age when they are diagnosed usually have chemotherapy for about 2 years. After that, your child might have a course of radiotherapy to help stop the astrocytoma from coming back.
Generally, chemotherapy treatment for low grade glioma can last up to a year to 18 months. But your child has most of their treatment on outpatient or daycare ward and can go home after. Many children return to school while having this type of chemotherapy treatment.
It’s difficult for doctors to predict how well chemotherapy will work. Chemotherapy works best at killing cells that are growing and dividing quickly. Low grade tumours are slow growing, so it might take some time to see them shrink.
Targeted cancer drugs are a newer type of treatment. They are grouped together as they work by ‘targeting’ the differences that help a cancer cell survive and grow. There are many different types of targeted drugs. These are grouped together depending on how they work. These groups include monoclonal antibodies, cancer growth blockers, drugs that block cancer blood vessel growth and PARP inhibitors.
Some children might have a targeted cancer drug as their treatment, but this is mainly being looked at in clinical trials. Some of the targeted drugs children might have include:
-
bevacizumab
-
dabrafenib
-
trametinib
Bevacizumab is a monoclonal antibody (MAB). It works by recognising and finding specific proteins in cancer cells. Bevacizumab targets a cancer cell protein called vascular endothelial growth factor (VEGF). This protein helps cancers grow blood vessels, so they can get food and oxygen from the blood. All cancers need a blood supply to be able to survive and grow.
Bevacizumab works by blocking this protein and stops the cancer from growing blood vessels, so it’s starved and can't grow.
Some children might have a targeted cancer drug called bevacizumab to treat low grade astrocytoma. They have this with a chemotherapy drug called irinotecan. They usually only have it after other treatment hasn’t worked.
Some children with low grade astrocytoma have a change ( ) in the BRAF gene. The BRAF gene makes a protein that affects how cancers grow and divide. Certain drugs that block the BRAF protein stop cancer growing and spreading, such as dabrafenib and trametinib.
) in the BRAF gene. The BRAF gene makes a protein that affects how cancers grow and divide. Certain drugs that block the BRAF protein stop cancer growing and spreading, such as dabrafenib and trametinib.
Your child might have dabrafenib and trametinib if they have the BRAF gene change and low grade astrocytoma. And they need treatment that reaches the whole body ( ).
).
Treatment for high grade astrocytoma
Your child might have:
Your child might have surgery to:
- remove all or as much of the tumour as possible
- take a piece of the tumour to look at under the microscope (a biopsy), to find out for certain what type of tumour it is
After surgery your child might have radiotherapy. They are likely to start treatment quickly after their surgery. Especially if they have lots of symptoms. Radiotherapy uses high energy x-rays to destroy any remaining cancer cells.
Doctors try to avoid giving radiotherapy treatment to children:
- under the age of 3 (this depends on where the tumour is)
- with NF1
This is because they are at higher risk of severe side effects during and after treatment. Doctors might reduce the amount (dose) of radiotherapy or delay it until your child is a bit older to try and prevent these side effects.
Research has shown that chemotherapy can help children with high grade astrocytoma. Children with high grade astrocytoma usually have chemotherapy for 6 to 12 months.
If your child is under 3 years of age, they usually have surgery and then chemotherapy. They may also have radiotherapy but this depends on where the tumour is.
For children over 3 years of age, they have surgery and then radiotherapy to the area. Some children may have chemotherapy alongside the radiotherapy. This is called chemoradiotherapy. In most cases children have more chemotherapy after their course of radiotherapy.
Research continues to look for the best chemotherapy drugs and length of treatment for high grade astrocytoma in children. Because of this, many children who have chemotherapy have it as part of a clinical trial.
Targeted cancer drugs are a newer type of treatment. They are grouped together as they work by ‘targeting’ the differences that help a cancer cell survive and grow. There are many different types of targeted drugs. These are grouped together depending on how they work. These groups include monoclonal antibodies, cancer growth blockers, drugs that block cancer blood vessel growth and PARP inhibitors.
Some children might have a targeted cancer drug as their treatment, but this is mainly being looked at in clinical trials.
Some children with high grade astrocytoma have a change ( ) in the BRAF gene. The BRAF gene makes a protein that affects how cancers grow and divide. Certain drugs that block the BRAF protein stop cancer growing and spreading, such as dabrafenib and trametinib.
) in the BRAF gene. The BRAF gene makes a protein that affects how cancers grow and divide. Certain drugs that block the BRAF protein stop cancer growing and spreading, such as dabrafenib and trametinib.
Your child might have dabrafenib and trametinib if they have the BRAF gene change and high grade astrocytoma. And your child has had treatment with radiotherapy or chemotherapy.
Astrocytoma that has come back
The treatment for a brain tumour that has come back depends on the first treatment that your child had.
Your child's surgeon may be able to operate again. If your child didn't have radiotherapy before, their specialist may suggest it now. If your child has had radiotherapy, they may still be able to have it again. Or their doctor may suggest chemotherapy instead.
Your child’s doctor might suggest they join a clinical trial if it has come back or not gone away with treatment.
Side effects
The side effects of treatment are different for each child. Some side effects of chemotherapy and radiotherapy happen during treatment and go away once treatment finishes. Other side effects, known as late effects or long term effects, happen months or years after treatment. These can be mild or more challenging. Not all children have challenging long term side effects.
A team of specialists closely monitors your child after treatment finishes. This is to help with any long term side effects.
The side effects of treatment might lead to problems at school or with your child meeting their developmental milestones. Many children have hormonal problems because of where the tumour was in the brain. Your child might have some physical disabilities or seizures after treatment.
We have detailed information on follow up and late effects of children’s brain tumour treatment, what treatments can help and where to get support. There is long term support available from a brain tumour late effects service.
Clinical trials
Doctors and researchers do trials to make existing treatments better and develop new treatments. They also want to find ways to reduce the side effects of treatment. Many children have their treatment for a brain tumour as part of a clinical trial.
Coping when your child has a brain tumour
We have information about where to get help and support when your child has a brain tumour.



